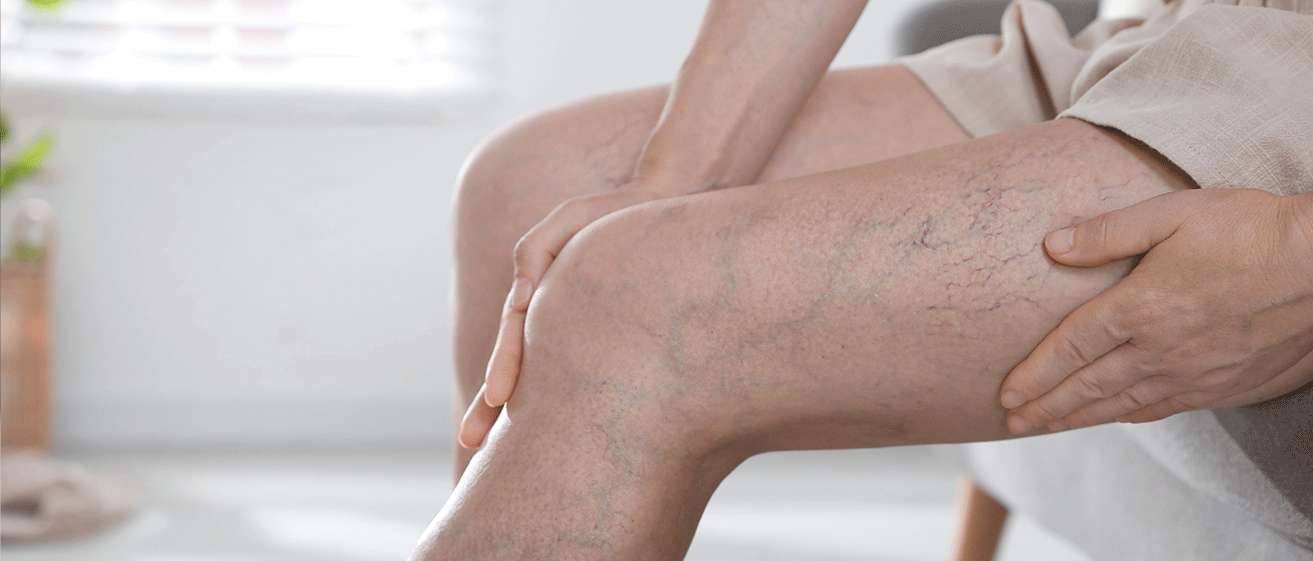

Varicose veins are commonly thought of as a cosmetic issue. Many people notice bulging or twisted
veins on their legs and assume they are harmless. However, it is natural to wonder whether varicose
veins could signal something more serious, and certain patients end up concerned about whether they
are dangerous.
The long-term effects of varicose veins can vary. In some cases, they remain a mild condition that
mainly affects appearance. In others, they may be linked to underlying vein problems that can lead
to pain, discomfort, swelling and changes in the skin over time. Understanding how these veins
affect your body can help you identify the potential side effects and seek out the necessary help.
What Are Varicose Veins?
Varicose veins are enlarged, twisted veins that commonly develop in the legs. They occur when the
valves inside the veins fail to work properly. Under normal conditions, these valves prevent blood
from flowing backwards and help move it upwards towards the heart. When the valves weaken, blood can
pool within the vein, increasing internal pressure. Over time, this causes the vein to stretch,
widen and become more visible beneath the skin.
Varicose veins typically affect the superficial veins of the lower limbs, which sit close to the
skin surface and are exposed to higher pressure from standing and walking. This ongoing strain can
contribute to valve dysfunction and vein wall weakness.
Why Do Varicose Veins Develop?
Varicose veins develop due to a combination of factors that affect vein structure and blood flow. The main underlying issue is chronic strain on the veins, particularly in the legs.
Several risk factors increase the likelihood of developing varicose veins:
- Age: As people age, their vein walls and valves gradually lose strength and elasticity, making it harder for blood to flow upwards against gravity.
- Genetics: A family history of varicose veins increases the likelihood of developing the condition.
- Gender and Hormonal Factors: Women are more commonly affected. Hormonal changes during pregnancy, menstruation and menopause can influence vein tone and blood flow.
- Pregnancy: Increased blood volume and pressure on pelvic veins during pregnancy can impair blood return from the legs.
- Body Weight: Excess body weight places additional pressure on the veins of the lower limbs.
- Work and Lifestyle Habits: Jobs or lifestyles that involve prolonged standing or sitting, such as retail work, teaching, healthcare or office-based roles, can increase strain on leg veins over time.
Possible Complications Associated with Varicose Veins
While some people live with varicose veins without significant issues, others may experience symptoms that gradually worsen. In certain cases, complications can develop, particularly when the underlying vein problem is not addressed.
Pain, Heaviness and Swelling
One of the most common problems associated with varicose veins is persistent leg discomfort.
Patients may describe aching, throbbing or a heavy sensation in the legs, especially after prolonged
standing or sitting.
Swelling around the ankles and lower legs may also occur. This is caused by increased pressure in
the veins, which allows fluid to leak into the surrounding tissue.
Skin Changes Around the Lower Legs
Long-standing vein problems can affect the skin. Poor blood return can lead to changes in skin colour, texture and sensitivity. The skin around the ankles and lower legs may become darker, dry or itchy. Some patients notice thickening or hardening of the skin in these areas.
Venous Eczema
Venous eczema is a form of skin inflammation linked to long-term vein disease. It usually appears as red, itchy, flaky or weeping skin on the lower legs. This condition occurs when fluid and inflammatory substances leak from poorly functioning veins into the surrounding skin.
Venous Leg Ulcers
One of the more serious complications of untreated varicose veins is the development of venous leg ulcers. These are open wounds that usually form around the ankles. They result from prolonged high pressure in the veins, which damages the surrounding tissues and reduces the skin’s ability to heal.
Blood Clots and Deep Vein Thrombosis (DVT)
Varicose veins are linked to a higher risk of certain blood clots, particularly superficial
thrombophlebitis, which occurs in veins close to the skin. These clots are usually not
life-threatening, but they can cause pain and swelling and may indicate more extensive vein disease.
In some cases, clots can also form in deeper veins, leading to deep vein thrombosis (DVT). DVT is
more serious and requires prompt medical attention. Although varicose veins do not always lead to
DVT, they may increase overall risk, especially in individuals with other contributing factors.
Can Varicose Veins Be Treated?
There are treatment methods for varicose veins. Initial measures to treat varicose veins include lifestyle management, such as regular movement, leg elevation and wearing compression stockings. When these methods do not manage symptoms, specialists can make use of modern varicose vein treatment to alleviate underlying vein problems.
Endovenous Laser Therapy (EVLT)
Endovenous Laser Therapy uses laser energy to close the affected vein. A thin laser fibre is
inserted into the vein through a small puncture in the skin. Once positioned, the laser delivers
controlled heat that causes the vein walls to collapse and seal shut.
Blood is then naturally redirected to nearby healthy veins. EVLT is commonly performed under local
anaesthesia and patients can usually resume normal activities shortly after the procedure.
Radiofrequency Ablation (RFA)
Radiofrequency Ablation is another minimally invasive treatment that uses heat to close the diseased vein. A catheter is inserted into the affected vein and radiofrequency energy is delivered through the device.
The heat generated by the catheter causes the vein to collapse and seal. RFA is often associated with minimal discomfort and a relatively quick recovery period.
ClariVein
ClariVein is a treatment that combines mechanical and chemical techniques to close the vein. A
specialised catheter with a rotating tip is inserted into the affected vein. As the catheter
rotates, a sclerosant solution is delivered into the vein.
The combined action irritates the vein wall and causes it to close. This method does not rely on
heat, which may reduce the need for multiple anaesthetic injections during the procedure.
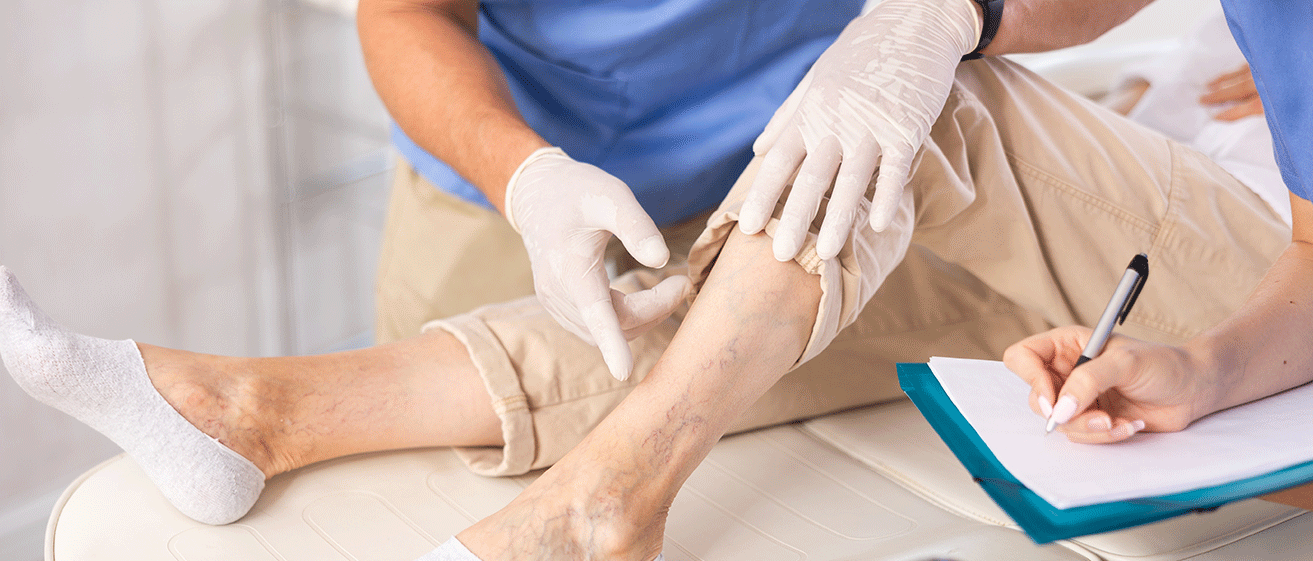
When Should You See a Doctor About Varicose Veins?
It is advisable to seek medical advice and treatment if varicose veins are associated with ongoing
symptoms or skin changes.
You should consider seeing a doctor if you experience:
- Persistent leg pain or swelling
- Skin discolouration or thickening around the ankles
- Itching, redness or eczema over varicose veins
- Bleeding from a vein
- Open wounds that do not heal
- Sudden leg swelling or pain
Varicose veins are not always dangerous, but symptoms should not be ignored. Over time, untreated
vein problems may lead to chronic discomfort, skin changes or complications that affect daily
activities and overall leg health.
At the Vascular & General Surgery
Centre, consultant vascular and general surgeon Dr Sujit Singh Gill
provides specialist treatment for venous disorders, including varicose veins. Dr Singh evaluates
each patient’s condition carefully and recommends treatment options based on the severity of the
symptoms involved. Early consultation can help identify potential complications and guide
appropriate management to improve both comfort and long-term vein health.
Contact us today to find
out more or schedule an appointment.




